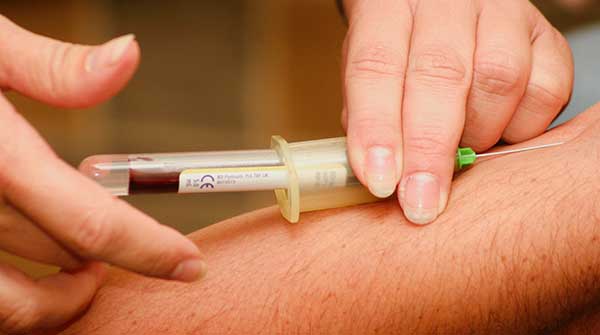
Simple blood test can predict who gets severe scleroderma and points the way to future treatments
A groundbreaking discovery by a cross-disciplinary research team at the University of Alberta may revolutionize the way scleroderma, a rare and debilitating autoimmune condition, is diagnosed and treated. The team has identified a biological marker, polysialic acid, that not only predicts the severity of the disease but also offers potential avenues for new therapeutic interventions.
Scleroderma, affecting approximately 17,000 Canadians, is characterized by an overproduction of collagen that leads to the hardening of the skin. In severe cases, it can also affect blood vessels and internal organs, resulting in a grim statistic: roughly 40 percent of patients succumb to the disease within five years of diagnosis. Although medication, diet, and exercise can help manage symptoms and slow progression, until now there has been no reliable method to predict who will develop the most severe form of the illness.
In their recently published research, the U of A team found that polysialic acid is elevated in both the skin and blood of patients with systemic sclerosis and correlates with the level of fibrosis. Polysialic acid, a glycan or sugar modification found on the surface of cells in the immune, reproductive, and nervous systems, has also been associated with aggressive cancer cells.
 Mohamed Osman |
 Lisa Willis |
Dr. Mohamed Osman, a rheumatologist, immunologist, and associate professor in the Faculty of Medicine & Dentistry at the University of Alberta, emphasized the importance of early identification in managing scleroderma: “Scleroderma is a terrible disease that starts with debilitating fatigue and then leads to systemic scarring. Imagine … feeling trapped in your own body. It’s key to identify those whose disease will progress because we want to be able to treat them early to minimize damage.”
The team’s blood test for polysialic acid, developed by co-principal investigator Dr. Lisa Willis, an assistant professor in the Faculty of Science and a glycans expert, offers a cost-effective and accessible diagnostic tool. “What you need for a biomarker is something that can be used cheaply in a clinic. We developed our test to be able to look for our molecule from the vial of blood that was already taken from a patient at diagnosis,” says Dr. Willis.
Although scleroderma is generally considered an inflammatory autoimmune disorder, it often does not respond to treatments that suppress the immune system. Some patients resort to stem cell transplants to replace non-functioning bonhttps://thegrizzlygazette.com/health/new-prostate-cancer-diagnosis-test-unveiled/e marrow, an expensive procedure costing approximately $80,000 per patient.
The researchers found that patients who had undergone bone marrow transplants showed reduced levels of polysialic acid, indicating a direct correlation between glycan changes and the disease process.
Despite not having worked together previously, Dr. Osman and Dr. Willis were drawn to the intriguing similarities between scleroderma and cancer. They hypothesize that the glycan may interfere with the body’s ability to combat scarring.
“Sugars form a really thick layer on the outside of a cell that is responsible for mediating the interactions between the cell and its environment. The sugars are what the immune system uses to say, ‘OK, this is self, I don’t want to attack this,’ or ‘This is foreign, I should deal with it.’ Normally, the immune system should recognize those pathogenic scleroderma cells, but the scleroderma cells make the glycan so they can grow without being killed,” explains Dr. Willis.
The researchers plan to further test the biomarker’s diagnostic potential by examining skin and blood samples from a broader cross-section of patients from across Canada and other parts of the world. Additionally, they aim to pinpoint the mechanism underlying these findings.
Dr. Osman envisions the research leading to a new avenue of treatment for scleroderma: “This is a paradigm shift – a potentially very important different way of looking at how to manipulate immune responses. As an immunologist, that’s very exciting.”
| Staff
The opinions expressed by our columnists and contributors are theirs alone and do not inherently or expressly reflect the views of our publication.
© Troy Media
Troy Media is an editorial content provider to media outlets and its own hosted community news outlets across Canada.